Periodontal disease is a chronic inflammatory condition that affects the tissues surrounding the teeth, including the gums, ligaments, and bone structures. It is characterized by the buildup of plaque, a sticky film of bacteria that forms on the teeth, leading to gum inflammation, bleeding, and eventual damage to the supporting structures. While periodontal disease is a well-known oral health concern, recent research has highlighted its potential impact on pregnancy outcomes.
Pregnancy is a critical period during which the health of the mother directly influences the well-being of the developing fetus. It is increasingly recognized that maternal oral health plays a significant role in overall pregnancy outcomes. The mouth serves as a gateway to the body, and oral conditions, including periodontal disease, have the potential to affect systemic health.
The connection between periodontal disease and pregnancy outcomes has gained attention due to mounting evidence suggesting a correlation between the two. Researchers have been exploring the mechanisms through which periodontal disease may influence pregnancy, and the findings are shedding light on the importance of oral health care during this crucial time.
This article aims to delve into the relationship between periodontal disease and pregnancy outcomes, emphasizing the need for heightened awareness and proactive management of oral health during pregnancy. By understanding the potential impact of periodontal disease on pregnancy, healthcare professionals can better educate pregnant women about the importance of maintaining good oral hygiene and seeking appropriate dental care.
The subsequent sections of this article will delve into the specifics of periodontal disease and its implications for pregnancy outcomes. It will explore the potential mechanisms that underlie the association between periodontal disease and adverse pregnancy outcomes, including preterm birth, low birth weight, and preeclampsia. Furthermore, the article will discuss strategies for managing and preventing periodontal disease during pregnancy, highlighting the role of regular dental check-ups, proper oral hygiene practices, and educational interventions.
Unveiling the Hidden Dangers: A Critical Examination of Periodontal Disease
Periodontal disease, also known as gum disease, is a chronic inflammatory condition that affects the tissues surrounding the teeth, including the gums, ligaments, and bone. It is primarily caused by the buildup of plaque, a sticky film of bacteria that forms on the teeth.
Plaque is constantly forming on the teeth, and if not removed through regular brushing and flossing, it can harden into tartar (calculus) within a matter of days. Tartar provides an ideal environment for bacteria to thrive, leading to the development of periodontal disease.
The progression of periodontal disease typically follows a series of stages:
Gingivitis: This is the earliest stage of periodontal disease and is characterized by inflammation of the gums. The gums may appear red, swollen, and may bleed easily during brushing or flossing. At this stage, the bone and connective tissues that hold the teeth in place are generally unaffected.
Periodontitis: If left untreated, gingivitis can progress to periodontitis. In this stage, the inflammation extends beyond the gums and affects the supporting structures of the teeth. Periodontal pockets form as the gum tissue pulls away from the teeth, creating spaces where bacteria can accumulate.

Preterm birth refers to the delivery of a baby before 37 completed weeks of gestation. Low birth weight, on the other hand, is defined as a baby weighing less than 2,500 grams (5.5 pounds) at birth. Both preterm birth and low birth weight are significant concerns in obstetrics, as they are associated with increased risks of infant morbidity and mortality.
The association between periodontal disease and preterm birth/low birth weight has been a subject of scientific investigation. Various studies have demonstrated a correlation between poor oral health, specifically periodontal disease, and an increased likelihood of delivering prematurely or having a baby with low birth weight.
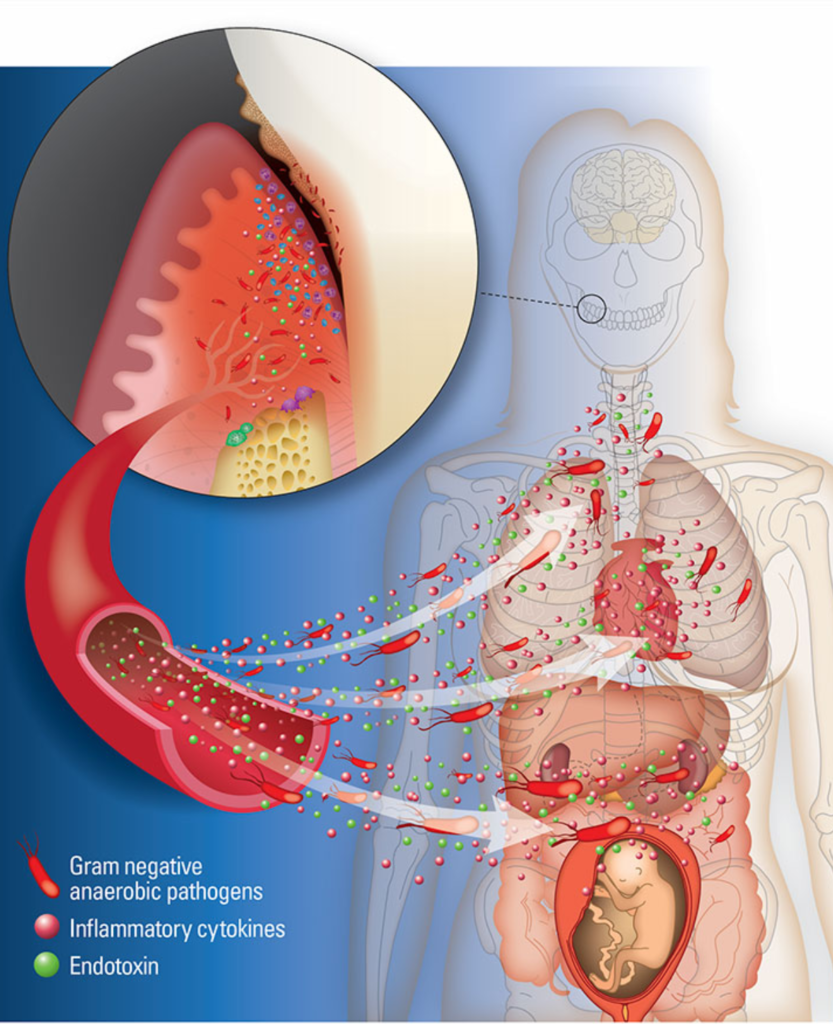
One proposed mechanism linking periodontal disease to adverse pregnancy outcomes is the translocation of bacteria from the oral cavity into the bloodstream. The bacteria present in periodontal pockets can enter the bloodstream through the inflamed gum tissue and travel to other parts of the body, potentially reaching the placenta. This bacterial invasion and subsequent inflammatory response can disrupt normal placental function and fetal development, leading to preterm birth and low birth weight.
Additionally, the systemic inflammatory response triggered by periodontal disease may play a role in these adverse outcomes. Chronic inflammation, which is characteristic of periodontal disease, can stimulate the release of pro-inflammatory mediators and cytokines. These inflammatory molecules can have systemic effects, potentially affecting the uterus and placenta, and contributing to the onset of preterm labor or impaired fetal growth.
Research studies have provided evidence supporting the association between periodontal disease and preterm birth/low birth weight. A meta-analysis combining data from multiple studies found that pregnant women with periodontal disease had a significantly higher risk of preterm birth compared to those without periodontal disease. The analysis also revealed that the odds of having a low birth weight baby were approximately two to three times higher among women with periodontal disease.
Given the potential impact on maternal and infant health, it is crucial to address periodontal disease during pregnancy. Routine dental care, including professional cleanings and proper oral hygiene practices, can help manage periodontal disease and reduce the associated risks. Identifying and treating oral health issues early in pregnancy, or ideally even before conception, is particularly important.
Preeclampsia is a pregnancy complication characterized by high blood pressure (hypertension) that usually develops after the 20th week of pregnancy. It is often accompanied by damage to other organs, typically the liver and kidneys. Preeclampsia affects approximately 5-8% of pregnancies and is a leading cause of maternal and fetal morbidity and mortality worldwide.
Symptoms of preeclampsia can vary, but commonly include:
In severe cases, preeclampsia can lead to life-threatening complications, such as:
The exact cause of preeclampsia is still not fully understood. However, it is believed to involve several factors, including:
Early detection and appropriate management of preeclampsia are essential for minimizing risks to both the mother and the baby. Prenatal care plays a crucial role in monitoring blood pressure, proteinuria, and other signs of preeclampsia. Treatment options may include:
Preeclampsia is a serious condition that requires close monitoring and medical intervention. Pregnant women should attend regular prenatal check-ups, be aware of the symptoms of preeclampsia, and report any concerns to their healthcare provider promptly. With proper management and timely intervention, the outcomes for both the mother and the baby can be improved.
In the United States, preeclampsia is a significant concern for maternal health. It is estimated that approximately 2-8% of pregnancies in the country are affected by preeclampsia. The condition contributes to maternal morbidity and mortality, as well as adverse outcomes for the baby.
Preeclampsia-related complications are a leading cause of maternal mortality in the United States. According to the Centers for Disease Control and Prevention (CDC), hypertensive disorders, including preeclampsia, accounted for 12.7% of pregnancy-related deaths between 2011 and 2016. It is worth noting that these deaths often occur during the postpartum period, emphasizing the importance of continued monitoring and care after delivery.
Recognizing the potential impact of periodontal disease on pregnancy outcomes, it is crucial to prioritize oral health during pregnancy. Regular dental check-ups and professional cleanings are essential, as they can help identify and treat any oral health issues promptly. Maintaining good oral hygiene practices, including brushing teeth twice daily, flossing, and using mouthwash, is also crucial.
Furthermore, education and awareness programs targeted towards pregnant women can promote the importance of oral health and encourage preventive measures. Healthcare providers should incorporate discussions about oral health into prenatal care, stressing the need for regular dental visits and proper oral hygiene habits.
The connection between periodontal disease and adverse pregnancy outcomes, including preterm birth, low birth weight, and preeclampsia, highlights the significance of oral health during pregnancy. By addressing periodontal disease through preventive measures and timely interventions, healthcare providers can potentially improve pregnancy outcomes and contribute to the overall well-being of both the mother and the baby. Promoting oral health awareness and integrating oral health into prenatal care should be an integral part of maternal healthcare strategies.